- Pendahuluan
- Patofisiologi
- Etiologi
- Epidemiologi
- Definisi Kasus dan Derajat Penyakit
- Diagnosis
- Penatalaksanaan
- Prognosis
- Edukasi dan Promosi Kesehatan
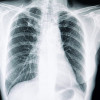
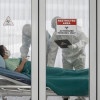
Penatalaksanaan COVID-19 (Coronavirus Disease 2019)
Penatalaksanaan COVID-19 (coronavirus disease 2019) bergantung pada tingkat keparahannya, yaitu tanpa gejala, derajat ringan, derajat sedang, dan derajat berat atau kritis. Pada pasien dengan gejala ringan, isolasi dapat dilakukan di rumah. Pada pasien dengan penyakit berat atau risiko pemburukan, maka dapat dilakukan rawat inap.[1,6,7]
Obat-Obatan yang Memiliki Efektivitas untuk COVID-19
Berdasarkan Living WHO guideline on drugs for COVID-19, terdapat obat-obatan yang direkomendasi kuat untuk diberikan kepada pasien COVID-19 (strong recommendations in favour), yaitu kortikosteroid dan IL-6 receptor blockers. Kedua obat ini digunakan pada pasien dengan keparahan berat dan kritis, sedangkan pasien gejala ringan tidak ada rekomendasi kuat.[7,27-29]
Referensi
1. Cascella M, Rajnik M, et al. Features, Evaluation, and Treatment of Coronavirus (COVID-19). Treasure Island (FL): StatPearls Publishing; 2023 Jan. https://www.ncbi.nlm.nih.gov/books/NBK554776/
6. Burhan E, Susanto AD, et al. Pedoman Tatalaksana COVID-19: Edisi 4. 2022.
7. World Health Organization. Therapeutics and COVID-19 Living Guideline. WHO. 2022 Jan 14. https://apps.who.int/iris/bitstream/handle/10665/351006/WHO-2019-nCoV-therapeutics-2022.1-eng.pdf
9. Forchette L, Sebastian W, Liu T. A Comprehensive Review of COVID-19 Virology, Vaccines, Variants, and Therapeutics. Current Medical Science. 2021;41(6):1037-1051. doi:10.1007/s11596-021-2395-1
10. van Doremalen N, Bushmaker T, et al. Aerosol and Surface Stability of SARS-CoV-2 as Compared with SARS-CoV-1. N Engl J Med. 2020.
19. Kemenkes RI. Situasi COVID-19. Kementerian Kesehatan RI. 2023. https://infeksiemerging.kemkes.go.id.
23. Kemenkes RI No. Hk.01.07/Menkes/4641/2021 tentang Panduan Pelaksanaan Pemeriksaan, Pelacakan, Karantina, dan Isolasi Dalam Rangka Percepatan Pencegahan dan Pengendalian Coronavirus Disease 2019 (COVID-19). Mei 2021. https://covid19.go.id/storage/app/media/Regulasi/2021/Mei/kmk-no-hk0107-menkes-46
27. World Health Organization. Therapeutics and COVID-19 Living Guideline. WHO. 2022 Jan 14.
28. Landolf KM, Lemieux SM, et alD. Corticosteroid use in ARDS and its application to evolving therapeutics for coronavirus disease 2019 (COVID‐19): A systematic review. Pharmacotherapy: The Journal of Human Pharmacology and Drug Therapy. 2022 Jan;42(1):71-90.
29. Wei Q, Lin H, et al. Tocilizumab treatment for COVID-19 patients: a systematic review and meta-analysis. Infectious diseases of poverty. 2021 Dec;10(1):1-7.
30. Tian J, Zhang M, et al. Repurposed tocilizumab in patients with severe COVID-19. The Journal of Immunology. 2021 Feb 1;206(3):599-606.
31. Rawat D, Roy A, et al. Vitamin C and COVID-19 treatment: A systematic review and meta-analysis of randomized controlled trials. Diabetes Metab Syndr. 2021;15(6):102324. doi:10.1016/j.dsx.2021.102324
32. Stroehlein JK, Wallqvist J, et al. Vitamin D supplementation for the treatment of COVID-19: a living systematic review. Cochrane Database Syst Rev. 2021 May 24;5(5):CD015043. doi: 10.1002/14651858.CD015043. PMID: 34029377; PMCID: PMC8406457.
33. Joshi S, Parkar J, et al. Role of favipiravir in the treatment of COVID-19. International Journal of Infectious Diseases. 2021 Jan 1;102:501-8.
34. Bosaeed M, Alharbi A, et al. Efficacy of favipiravir in adults with mild COVID-19: a randomized, double-blind, multicentre, placebo-controlled clinical trial. Clin Microbiol Infect. 2022 Apr;28(4):602-608.
35. Shinkai M, Tsushima K, et al. Efficacy and Safety of Favipiravir in Moderate COVID-19 Pneumonia Patients without Oxygen Therapy: A Randomized, Phase III Clinical Trial. Infect. Dis. Ther. 2021;10:2489–509.
36. Butler CC, Hobbs FDR, et al. Molnupiravir plus usual care versus usual care alone as early treatment for adults with COVID-19 at increased risk of adverse outcomes (PANORAMIC): an open-label, platform-adaptive randomised controlled trial. Lancet. 2023 Jan 28;401(10373):281–93.
37. Pfizer. Pfizer’s novel COVID-19 oral antiviral treatment candidate reduced risk of hospitalization or death by 89% in interim analysis of phase 2/3 epic-hr study. 2021. https://www.pfizer.com/news/press-release/press-release-detail/pfizers-novel-covid-19-oral-antiviral-treatment-candidate
38. Wang L, Berger NA, Davis PB, et al. COVID-19 Rebound After Paxlovid and Molnupiravir During January-June 2022. Preprint. medRxiv. 2022;2022.06.21.22276724. doi:10.1101/2022.06.21.22276724
39. Marovich M, Mascola JR, Cohen MS. Monoclonal Antibodies for Prevention and Treatment of COVID-19. JAMA - J Am Med Assoc. 2020;342(2):131–2.
40. Izquierdo-Alonso JL, Pérez-Rial S, et al. N-acetylcysteine for prevention and treatment of COVID-19: Current state of evidence and future directions. J Infect Public Health. 2022 Dec;15(12):1477-1483. doi: 10.1016/j.jiph.2022.11.009. Epub 2022 Nov 12. PMID: 36410267; PMCID: PMC9651994.
41. Ader F, Bouscambert-Duchamp M, et al. Remdesivir plus standard of care versus standard of care alone for the treatment of patients admitted to hospital with COVID-19 (DisCoVeRy): a phase 3, randomised, controlled, open-label trial. Lancet Infect Dis. 2021 Sep 14:S1473-3099(21)00485-0.
42. The RECOVERY Collaborative Group. Dexamethasone in Hospitalized Patients with Covid-19. N Engl J Med. 2021;384(8):693–704.
43. Kang S, Tanaka T, Kishimoto T. Therapeutic uses of anti-interleukin-6 receptor antibody. Int Immunol. 2015;27(1):21–9.
44. Chen CX, Wang JJ, et al. JAK-inhibitors for coronavirus disease-2019 (COVID-19): a meta-analysis. Leukemia. 2021;35(9):2616-2620. doi:10.1038/s41375-021-01266-6
45. Tzilas V, Manali E, et al. Intravenous Immunoglobulin for the Treatment of COVID-19: A Promising Tool. Respiration. 2021;99(12):1087–9.
46. Aliyu B, Raji YE, et al. Systematic review and meta-analysis of the efficacy and safety of oseltamivir (Tamiflu) in the treatment of Coronavirus Disease 2019 (COVID-19). PLoS One. 2022 Dec 1;17(12):e0277206. doi: 10.1371/journal.pone.0277206. PMID: 36454880; PMCID: PMC9714710.
47. Bleyzac N, Goutelle S, Bourguignon L, Tod M. Azithromycin for COVID-19: More Than Just an Antimicrobial? Clin Drug Investig. 2020;40(8):683–6
48. Okumuş N, Demirtürk N, et al. Evaluation of the effectiveness and safety of adding ivermectin to treatment in severe COVID-19 patients. BMC Infect Dis. 2021;21(1):1–11.
49. Chiu L, Lo CH, et al. Colchicine use in patients with COVID-19: A systematic review and meta-analysis. PLoS One. 2021 Dec 28;16(12):e0261358. doi: 10.1371/journal.pone.0261358. PMID: 34962939; PMCID: PMC8714120.
50. Jiang F, Deng L, et al. Review of the Clinical Characteristics of Virus corona Disease 2019 (COVID-19). J Gen Intern Med. 2020;2019:1–5.
51. Santamarina MG, Beddings I, et al. Sildenafil for treating patients with COVID-19 and perfusion mismatch: a pilot randomized trial. Crit Care. 2022 Jan 3;26(1):1. doi: 10.1186/s13054-021-03885-y. PMID: 34980198; PMCID: PMC8721481.
52. Reis S, Popp M, eta l. Anticoagulation in COVID-19 patients - An updated systematic review and meta-analysis. Thromb Res. 2022 Nov;219:40-48. doi: 10.1016/j.thromres.2022.09.001. Epub 2022 Sep 8. PMID: 36113402; PMCID: PMC9451936.
53. Lenze EJ, Mattar C, et al. Fluvoxamine vs Placebo and Clinical Deterioration in Outpatients With Symptomatic COVID-19: A Randomized Clinical Trial. JAMA. 2020;324(22):2292–2300.
54. Sasaki M, Tabata K, et al. Oral administration of S-217622, a SARS-CoV-2 main protease inhibitor, decreases viral load and accelerates recovery from clinical aspects of COVID-19. bioRxiv. 2022 Jan 1.
(Konten ini khusus untuk dokter. Registrasi untuk baca selengkapnya)